The information given in this booklet may answer some questions you have and provide you with an understanding into what has happened throughout your stay in Critical Care. This booklet may also provide you with simple suggestions on how to resolve common issues patients have had after critical illness.
It is designed not only for you as a patient, but your family too. Critical illness is often unexpected and it is normal to feel emotionally unprepared and stressed about what has just happened. Often both patients and families find it hard to come to terms with the impact critical illness can have.
This booklet, along with your Critical Care diary will allow you to piece your journey together and assist you with the recovery process.
On this page
What is the Critical Care Department and why did I need to go?
Critical Care is an area within the hospital that cares for patients who are very unwell. You will have been admitted to this area because one or more of your organs were not working properly and required support. Due to the specialist treatments and higher level of support you need on Critical Care there are many more staff than you would see on a general ward. Our sickest patients are looked after on a one to one ratio and, the staff who look after you are trained to care for severely ill patients.
Family members may describe to you how unwell you were during this time, but it may be difficult for you to understand the severity of your illness. Below is a picture of a typical bed space within Critical Care. Surrounding the bed are machines that are often required when patients are unwell, some of these may have been used during your care.
This equipment may seem overwhelming or frightening but every item helps the staff monitor you closely. You may remember hearing alarms, on most occasions the machines are simply drawing the attention of the nurse to check your condition.
If you would like more information on what happens in Critical Care please visit: www.icuunwrapped.co.uk
This website was written by members of the Critical Care team at the Leeds Teaching Hospitals and seeks to inform and support both family and patients to understand Critical Care. It may help clarify your experiences.
Critical Care Diaries
When you were first admitted to Critical Care your family and friends will have been given a diary and encouraged by staff to fill it in on a daily basis. This allows your family to document procedures, surroundings, their feelings and thoughts at the time, events both in hospital and at home and importantly, progress you have made.
Often when patients are admitted to Critical Care they are sedated. When patients regain consciousness it is common not to remember what has happened or how unwell they have been. We hope that the diary will tell a story of what has happened to you whilst you were in Critical Care.
Transfer to the Ward
The decision for you to leave Critical Care is made by the consultants within Critical Care; you will only step down to the ward if the consultant feels it is appropriate to do so. Information will be shared with the team in the clinical area that you will be moving to regarding what happened during your stay on Critical Care.
Leaving Critical Care is a big step and although staff within Critical Care will prepare you for what is going to happen, you will find a significant difference between the levels of care you receive on Critical Care and the general wards.
The changing environment
Although Critical Care can be a challenging environment to be in, often patients who have had a long stay within Critical Care find it a ‘safe’ place to be. Within Critical Care staff are easily visible at all times, whereas on the ward this is not always be the case.
Transfer to the ward can be very worrying time for you and your family. Whist in Critical Care your family will be receiving regular updates on your condition and progress and when you move to the ward this may not be the case. The higher ratio of patients to staff may mean you have to wait longer for staff to be available for you to speak to and they may not be able to provide you with as much of their time to discuss treatment as the staff on Critical Care did.
Planning your recovery
When you leave Critical Care, a group of specialist nurses called Outreach will be made aware of your discharge. This team is made up of senior nurses who have advanced clinical skills and experience. They will work with you to rehabilitate you to the best of your ability.
The Critical Care Rehabilitation Team will also visit you once you have been discharged to the ward, they will work with you to try and restore you back to your pre admission condition. The rehab team will continue to visit you until you are discharged from hospital.
The aim of the Rehabilitation Team is to promote independence in areas that you are struggling with following your critical illness- This might be with hygiene and dressing needs, nutritional needs, mobility issues and any psychological problems that you may have. The Rehabilitation Team will support you throughout your recovery and are here to answer any questions you may have.
Recovery from illness is often the hardest part; the aim of the Rehabilitation Team is to promote your independence. When you are transferred to the ward the rehab team will encourage you to be more independent. Having to re-learn how to do simple things such as walking, eating, drinking or even breathing for yourself is normal after clinical illness. This can be frightening but the team will support you at every step of the way.
As you improve you will be encouraged to do things independently and often this can be very tiring. Setting small realistic goals on a daily basis can really help you achieve goals.
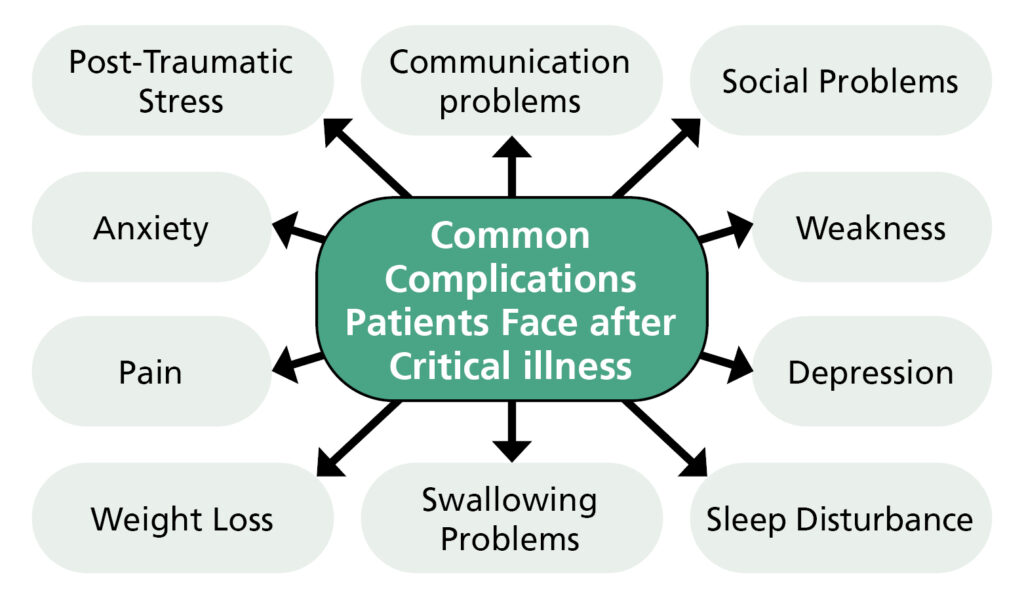
Getting back to your normal self
Your body and mind will have a lot of work to do to get back to normal, this will take time. There are several important things that you can do to help yourself recover:
Physical Activity
Our aim is that your recovery process will be tailored to meet your needs; the physiotherapy team will work with you to achieve this.
It is really important to do a little physical activity each day, walking up and down stairs, out in the garden or just round the block. Trying to push yourself further every day will really help you to see improvement.
Physical activity will keep your circulation active, help with muscle strengthening, build up your energy levels and help you feel more positive.
Rest and relaxation
Although you’re encouraged to get up and move about, rest and relaxation are also really important too. Your body does a lot of repair whilst your sleeping, don’t worry if you get tired easily, especially in the early stages (this is perfectly normal) it’s your bodies way of persuading you to rest.
Healthy diet
A balanced diet is an essential part of your recovery, however it is really important to enjoy what you eat and drink. Eating well means you will be able to fight off infection better and feel less weak and tired.
Eating normally again
The body responds in very specific ways during critical illness, because you use so many calories when you are poorly the body needs a much more nutrition to run effectively.
The body uses up its own resources such as muscle and fat to help you get better. This makes you weak because your muscles may have wasted, you may notice that your muscles are not as bulky as they were before.
Unfortunately it takes quite a bit of work to get the muscles back to normal.
Tips
- Eat small meals
- Take advantage of times when you feel hungry
- Take your time eating
- High protein drinks such as fortisip, complan and build up
Sometimes you may feel hungry and want to eat lots, but unfortunately the first thing that’s happens is we put fat back on before anything else.
It can take up to a year to get back to your normal weight, reduce fat and gain muscle; the critical care rehabilitation team will help you create achievable goals to do this.
Some people may find that your sense of taste has changed its common to have heightened or different tastes after a stay in critical care. These taste changes should only be temporary and should return to normal within a few weeks/months.
Sex after critical illness
Your illness may have reduced your sex drive and you or your partner may be concerned that sex could be harmful for you. You will be able to return to your normal relationship but recognise that this may take some time and patience from both of you- do only what you feel comfortable doing.
A small number of people may experience genuine medical problems such as impotence in men or dryness for women, your G.P’s can help you with these and as time progresses things may settle.
Women’s menstrual cycles may be sporadic following critical illness but ensure you continue to use contraception – your oral contraceptive may have been stopped whilst in hospital please check with your doctor before re starting it.
And don’t forget the power of small signs of affection, kissing and cuddles are really important. Most people find it hard to talk about sex, but just try and relax and a keep a sense of humour – Lots of people survive critical illness and it’s important to get back to normality.
Psychological changes in you
Anxiety
Anxiety after critical illness is understandable and normal. When you are worried, scared or in danger the stress response for your body is to produce chemicals to help you cope. The main chemical involved is adrenaline; frightening events, words, thoughts or memories that you may have from Critical Care will cause the body to produce adrenaline. There is nothing wrong with this it is nature’s way of helping you to cope with danger, if you were in real danger you might not notice the effects on your body.
The problems start when you have worrying thoughts but cannot respond in a physical manner – The adrenaline gets our body ready to respond and if it doesn’t get used up it may cause unpleasant physical and mental symptoms such as:
- Sleep deficiencies – your thoughts are racing – you struggle to relax- therefore you struggle to sleep
- Breathing difficulties- you may start breathing quicker- oxygen then floods your brain- making you feel dizzy or faint
- A racing heart
- Butterflies or a sinking feeling in your tummy
- Shut down the blood to your hands and feet- you may notice they feel cold and clammy
- Cold sweats
Depression
Felling in low spirits is very common after being critically ill, for most people these feelings in time will pass as you start to recover. (Be aware that much like your physical health it may take up to a year to feel back to your normal self). However if you continue to experience low mood so much so that it interferes with your day to day life we advise that you seek help from a health professional.
Signs and symptoms of Depression include:
- Signs and symptoms of Depression include:
- Sadness, either all the time or sometimes just out of the blue
- Tearfulness
- Loss of interest
- Loss of appetite
Delirium
You may experience these feelings and been distressed by how you acted or felt the rehab team can help you understand this.
Nightmares and Memories
Patients who have been critically unwell often report having nightmares whilst in intensive care or just after they leave. They may feel very real and often have been described as frightening. Much like other symptoms discussed in this booklet, usually these subside over the coming weeks or days as you get better.
Similarly hallucinations or panicky feelings that you may have are very common amongst patients leaving the critical environment. Being critically unwell and spending time on a Critical Care unit is something only a small fraction of society will experience in their lifetime. The reactions that you are having are your brains way of trying to piece together what has just happened and make sense out of the situation.
Talking things through will really help, whether it is with a family member, the rehab team, a member of ward staff or whoever you feel comfortable with.
Lifestyle changes
Smoking
If you smoked before you were unwell now is the perfect time to give up. For patients that have been seriously ill on intensive care, it’s important that you stop smoking because your lungs may have been affected by the illness. You may not notice the damage to your lungs but stopping smoking allows your lungs to recover.
Help with stopping smoking:
For Advice: www.nhs.uk/smokefree
Stop Smoking Clinics: Available on the NHS, They have a good success in helping people to stop smoking. Your Doctor can refer you to one if you’re keen to stop but are finding it difficult
Alcohol
The UK recommendation is that both men and women should drink no more than 14 units per week; this is equivalent to 6 glasses of 13% of 175ml of wine, 6 pints of 4% Beer or 14, 25ml shots of 40% spirits. It is suggested that you have at least two alcohol free days a week.
The more you drink above these limits, the greater the risk of developing serious problems, to find out more on this please speak to a health professional.
Support services
Three to six months after you have been discharged from hospital you will be invited to attend a follow up clinic, this is run by the medical and nursing staff from the Critical Care units. This will give you the opportunity to discuss retrospectively your experiences on Critical Care.
When you are in hospital staff will talk to you about what has happened throughout your time in Critical Care but it may not always ‘go in’. Some patients feel the follow up clinic gave a more detailed understating of what has happened during your time on Critical Care.
Many people value the opportunity to ask questions and note that the consultation was a good occasion to discuss what they’d remembered of their hospital experience, their dreams and hallucinations, physical and emotional recovery, any concerns, and to gain reassurance. Some also use it to discuss aspects of their care they’ve been unhappy with.
Regional Post Critical Care support group
The Leeds Teaching hospitals have a Regional Post Critical Care support group where ex ICU patients can meet and share experiences once a month, in a non-clinical environment. Please email: [email protected] for more information.
Further information and support
Health talk
This is a website supported by the NHS providing information for patients by patients who have been in intensive care. www.healthtalk.org/intensive_care
Intensive Care Society
Helps you find information about each step of a patient’s treatment and recovery from critical illness for both patients and relatives. www.ics.ac.uk/icf/patients-and-relatives
British Association for counselling and psychotherapy
This website explains what counselling and therapy are; It will also help you find counsellors and therapists in your local area. www.itsgoodtotalk.org.uk
ICU Steps
Patient Charity and Support group for people who have experienced critical illness. The website contains booklets, information and support boards. www.icusteps.org
West Yorkshire Critical Care Operational Delivery Network (wyccn.org)
IAPT – Better access to Psychological therapies through the NHS.
https://www.wyccn.org/patient-information.html
IAPT- Better access to Psychological therapies through the NHS
NHS England » Adult Improving Access to Psychological Therapies programme.
https://www.england.nhs.uk/mental-health/adults/iapt/
Get Self Help
Useful and free self-help material, including therapy techniques. www.getselfhelp.co.uk
Age UK
Age UK promotes the wellbeing of all older people. www.ageuk.org.uk
PALS (Patient Advice Liaison Service)
- Provides advice and support for patients, their families and carers
- Information on the NHS services to help you make choices
- Listen to your questions, suggestions, concerns and complaints
- Help sort out any problems you may have on your behalf
They can be contacted on by:
Phone: 0113 206 5261
Email: [email protected]
Research in critical care
The NHS recognises that patients should have the opportunity to participate in Research which will help to improve treatment and care for future patients in ICU.
While you were unwell in Critical Care, you were too unwell to give your permission to be involved in Research. Therefore your relative/friend/partner/doctor gave consent for you to take part in a Clinical Trial.
Consequently while you are recovering on the ward if you have been a research participant you will be approached by one of the Research Team to obtain your permission to continue to be involved in the trial. If you decide to decline this will not affect any future care you may receive and your decision will be respected.
However if you would like to discuss your involvement in a trial please feel free to contact the team;
Adult Critical Care Research contact number: 0113 206 9213