This booklet has been written to help you understand the purpose and method of freezing eggs. We hope that it will answer some of the questions that you may have.
We recognise that undergoing transition from one gender to another presents many challenges, including the potential to have your own genetic children in the future. Thinking about having children may not be a high priority right now. However, considering this now may allow you the opportunity to have children in the future.
Having your own genetic children may not be possible, or the chances reduced if you do not consider freezing your eggs before starting hormone drugs that can affect the quality of your eggs and /or before irreversible gender-affirming surgery. We will help you to make the right decisions for you as sensitively as we can.
Why am I being asked to consider storing my eggs?
For those assigned female at birth, you have been born with two ovaries containing a million of eggs. These are all the eggs you will ever have. They reduce in number as you get older, until about the age of 50 years when they have all gone. This is known as the ‘menopause’ and coincides with when a woman’s periods stop.
An egg contains half of the building blocks, or genetic material needed to develop into a baby. To make a baby the egg needs to join with a sperm to complete the building blocks that are needed.
You are considering taking, or have already started, medications that will lead to the transition from your birth gender to the gender you identify with. The types of medications used for gender transition could reduce your own natural chance of having children (fertility). It is difficult to know exactly what the effect of your treatment will be, and fertility may therefore be temporarily or permanently affected. Depending on the type of treatment and the duration of time you have taken the medications. Both ‘blockers’ (gonadotrophin releasing hormone agonists e.g. Gonapeptyl / Decapeptyl) and cross-sex hormones e.g. testosterone (the hormone usually produced from the testis) switch off the pituitary gland (in the brain) which turns off the hormonal signal to the ovaries and prevents development of egg containing sacs and release of eggs after maturing.
The best time to store eggs is before any medication (‘blockers’ or cross-sex hormones) is started, but it is possible to stop any of the transition medications to attempt to store eggs or achieve a pregnancy at any time.
You may need to be off these medications for several months to allow the natural cycle pattern to return in the ovary. Unfortunately, there are no guarantees that normal function will be restored.
We do not know completely what the long-term effects of testosterone treatment on the quality of the eggs might be, and this may make it harder to achieve a pregnancy. We also do not have much information about health of children born from eggs that have been exposed to high levels of testosterone.
Freezing eggs gives you the option to try to have genetically- related children in the future. This is not to say that other ways of having a family cannot be equally rewarding such as using donated gametes (egg or sperm), adoption or fostering. If gender-affirming surgery has not taken place, some people choose to stop their transition medication in the future to try for a natural pregnancy themselves, accepting that some female characteristics will temporarily return.
How is it done?
After puberty, production of FSH and LH hormones make the ovaries produce mature eggs (one per month). FSH and LH are released from the pituitary gland, situated in the base of the brain, into the blood stream to stimulate egg development and release of an egg each month.
By giving additional hormones, like in IVF, it is possible to make the ovary produce around 10-15 eggs at the same time with extra hormone treatment.
Taking GnRH analogues (‘blockers’) or testosterone will stop FSH and LH release from the pituitary gland, and as a result the eggs will not mature. This will also stop oestrogen hormone production from the ovary and hence the womb lining will not thicken.
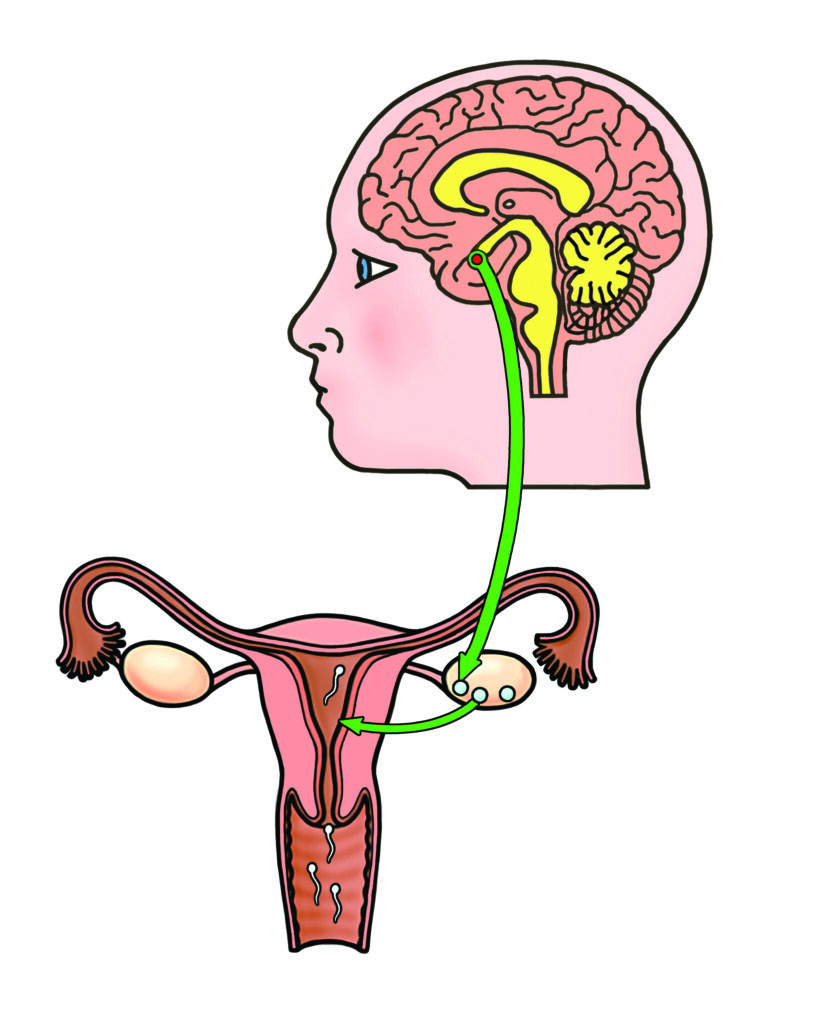
This is done with small injections into the skin of the tummy or thigh over 10-14 days.

You will need at least one vaginal (internal) ultrasound scan to determine when your eggs appear ready to take out and freeze.
The procedure of egg collection takes about 30 minutes. The eggs come out through a needle that goes through the skin inside the vagina. During the procedure you will have sedating medication and pain relief given through a drip in your vein.
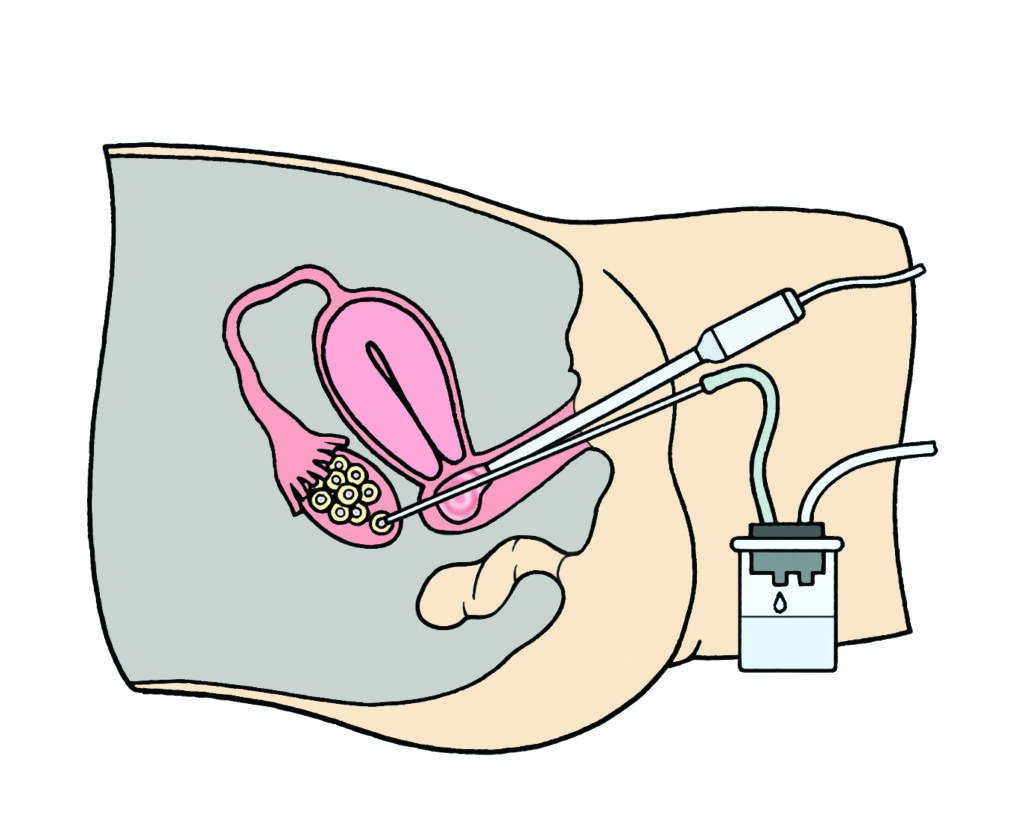
After your eggs have been taken out an embryology scientist will separate them from all the cells attached to them and process
them for freezing.
The eggs then undergo a process called vitrification (fast freezing) and are stored in tanks of liquid nitrogen, until the time is right for you to think about having a baby.
Most people will feel drowsy after the procedure, but you will be able to go home the same day. Any discomfort is easily managed with simple painkillers, and you will quickly improve over the next couple of days. A condition known as Ovarian Hyperstimulation Syndrome (OHSS) may make you feel poorly for longer if a lot of eggs have been frozen. Sometimes this means you need to stay in a hospital for a few days for monitoring and treatment.
There is a very small risk of excessive bleeding (less than one in 500 procedures), infection (less than one in 500 procedures) and damage to other structures inside your abdomen, such as bladder or bowel, which would require further treatment. Occasionally, there may not be many or any eggs suitable for storage.
More information will be provided about this process, and the future use of the eggs, if you would like to find out more.
Please note
After your initial assessment, you will be referred from Leeds Centre for Reproductive Medicine to CARE Fertility Leeds at Seacroft Hospital, Leeds where these procedures will be undertaken.
What happens next if I decide to freeze eggs?
- You must be 21 years or older for Leeds Centre for Reproductive Medicine to be able to offer eggs freezing for you. If you are under 21, we will be pleased to talk to you about the process for when you are old enough.
- You will be referred to Care Fertility Leeds once the initial assessments and investigations are complete.
- You will need to have a blood test to screen for infections (including Hepatitis B / C / HIV / Syphilis) as Care Fertility Leeds can only provide storage for people who do not have these infections. Further tests may be required depending on the future use of your eggs and Care Fertility Leeds will advise you appropriately.
- When the time is right to store your eggs (depending on your stage of transition and time off your medication) you may be asked to stop transition medications for a time.
- You will need to sign the required agreements (consent forms).
- You will be taught how to give the injections, when to start them and when to book an ultrasound scan to see how the ovaries are responding. You may need to have a few vaginal scans before the egg collection is planned.
- On the day of egg collection, you will attend Care Fertility Leeds early in the morning. You will see an anaesthetic doctor and the clinician who will collect your eggs.
- After the procedure and before you go home, you will find out how many eggs were collected and the number of eggs that were frozen.
- The eggs will be stored in the long-term storage freezer container at Care Fertility Leeds.
What happens when I want to use the eggs?
When you want to discuss using the stored eggs, you should request a referral to Leeds Centre for Reproductive Medicine from your GP. Any issues that have arisen with your health or well-being since your initial contact with us will be discussed. We will also talk you through the chances of your eggs surviving after being frozen and thawed which is approximately 95%.
We will explain how the eggs may be used and the chances of having a baby with them. How the eggs are used will depend on the type of relationship you are in and whether
gender-affirming surgery has been completed.
Please note
Before the egg has been in storage for 10 years you will need to be seen at Leeds Centre for Reproductive Medicine to confirm that your sample can continue to stay in storage. This is a legal requirement that the clinic must do.
If you have a female partner, the eggs could be fertilised using donated sperm to create embryos (earliest stage of a baby) before being put into your own womb (if you have not had the surgery to remove womb) or your partner’s womb or in a surrogate (somebody who carries a pregnancy for you in their womb) depending on your circumstances and wishes.
If you have a male partner, sperm from your partner can be used to create embryos using your frozen eggs, but you will need to consider using a surrogate.
The clinician will also advice you about fertility treatment options if you wish to have children as a single parent or if your partner is a trans or non-binary individual.
These are sensitive choices and will need to be carefully thought about by you and your partner (if you have one then). A session with a fertility counsellor will be required.
Currently, on an average just over one in four IVF treatments where an embryo is transferred to the mother results in a pregnancy. This is likely to get better in the future. For those people who use frozen eggs, the success rate is thought to be nearly the same, once those eggs have been fertilised.
What happens if I don’t ever want to use my eggs?
If you decide that you are never going to want, or be able to use your eggs, we expect you to advise Care Fertility Leeds and Leeds Centre for Reproductive Medicine to discard them.
We can discuss this with you at any time but also expect you to keep in regular contact with Care Fertility Leeds and Leeds Centre for Reproductive Medicine. Together with your transition doctors, we may advise you to discard your eggs in the future if you have completed your family or decide to stop the transition process.
Who pays for my egg freezing?
At the beginning, the NHS may fund the hospital appointments and egg freezing process, but this depends on your local health authorities (Integrated care boards or ICBs). As per the current local policy in West Yorkshire you must be receiving NHS England funded gender transition hormone treatment to allow the NHS to fund procurement and freezing of eggs for an initial 10 years.
If you do not meet the criteria for NHS funded egg freezing, in exceptional cases, an individual funding request (IFR) can be made by your GP or the specialist on your behalf. If this is not successful you will have the option to pay for it yourself. Please visit Care Fertility Leeds website for the current charges if you are interested.
It is important to realise that if you wish to use the stored eggs in the future, the fertility treatment required may not be paid for by the NHS, as different rules apply for NHS funded fertility treatment using frozen eggs. For example, there is currently no funding in Yorkshire and Humber region for fertility treatment as a single parent.
How long can my eggs be stored for?
The Law allows your eggs to be stored for 55 years from the date of first storage if you renew your consent to storage every 10 years.
What happens if I don’t want to freeze my eggs?
This is your decision to make with the support of those close to you and us if needed. Nothing will change in your transition journey if you decide not to freeze any eggs.
We can still see you at a future time if you wish to explore your fertility options again.
Is there anyone else I can talk to?
We know there is a lot of information to take in. Some people find it helpful to talk to someone who is not a close family member, friend or doctor / nurse involved in their treatment about how they feel and the decisions they are being asked to take.
Fertility counselling is currently not available at Leeds Centre for Reproductive Medicine, but appropriate information can be given if you wish to access counselling privately.
Important legal information
Storage of eggs for your own use
The following information is for your guidance. For further information please refer to the Human Fertilisation and Embryology Authority (HFEA)
- Your right to confidentiality under the HFE Act of parliament prohibits the normal exchange of information between clinicians without specific written consent unless it is deemed necessary for your continuing medical care.
- Before consenting to the storage of eggs you will receive verbal and written information and may wish to receive further counselling regarding the implications of taking the proposed steps.
- Anyone consenting to storage of their eggs must give their consent in writing prior to the storage.
Consent
The consent must specify one or more of the following:
- Whether the treatment is provided for yourself, or yourself and a named partner.
- Whether any eggs obtained can be used for research.
- The legal maximum period of storage is 55 years at 10 yearly increments.
- What is to be done with the eggs in the event of your death or if you become incapable of changing or withdrawing your consent. This is a legal requirement.
A. You may request that they are allowed to perish.
B. You may donate them for research.
C. Your named partner could be able to use them. If your female partner wishes to use your stored eggs, you must have nominated that person beforehand, in writing. Without your consent, your partner will not be able to use them.
D. You cannot donate your eggs for the treatment of anyone else.
We hope that this provides you with all the information needed. You are welcome to ask questions that arise during the course of reading this booklet.
Glossary
- Eggs: A woman’s lifetime supply of eggs is present in the ovary at birth. They reduce in number and quality with time. They pass on the half of the genetic instructions to the embryo/baby.
- Embryo: Once the egg is fertilised with sperm, it begins to cleave (multiply its cells) and is called an embryo.
- Fertilisation: Fertilisation is when the genetic material from the egg and sperm combine to create a new and unique cell which may go on to develop into an embryo and then a baby.
- FSH: Follicle stimulating hormone causes the eggs to mature in the ovary.
- GnRH agonist (‘Blocker’): A hormonal drug that first stimulates and then inactivates the pituitary gland e.g. Prostap, Buserelin; these can be used to block ovulation and oestrogen production.
- Gonadotrophins: Hormones produced naturally by the pituitary gland to stimulate the ovary to produce and release eggs and the testes to produce sperm e.g. FSH, LH. These drugs are produced as medicines to over-stimulate the ovary during IVF / egg freezing to get lots of eggs ready at once e.g. Merional, menopur, Gonal F.
- ICB: An Integrated Care Board decides on how treatment should be funded in local areas.
- Oestrogen: This hormone is naturally produced by the follicles in the ovary as the egg is growing. Its main job is to thicken the lining of the womb for a pregnancy to implant.
- OHSS: Ovarian hyperstimulation syndrome is a risk of hormonal stimulation of the ovaries. It can be serious if not recognised and treated. It happens when the ovaries are over-sensitive to the stimulation (FSH) injections and produce too many follicles. It can cause pain, abdominal bloating, sickness, diarrhoea, dehydration and rarely, serious blood clots. You will be warned if you are at risk, for the symptoms and signs to look out for and report to us for further advice.
- Ovary: Stores all the woman’s eggs for her whole life and produces hormones.
- Pituitary gland: A small gland situated in the base of the brain in the head, behind the nose, and produces many hormones including those that control the ovary and testis.
- Sperm: The sperm develop in testes and continue to do so throughout adult life. They do not suffer the same deterioration with age as eggs, as they are constantly being replaced. They pass on half of the genetic instructions to the embryo / baby.
- Surrogate: A woman who carries a pregnancy in her womb for another person.
- Testis: Where sperm production and storage takes place.
- Testosterone: The hormone mainly produced from the testes, that helps give male features e.g. facial hair, deeper voice whilst being involved in sperm production.